Dental X-Rays. Clarifications from the ODQ
A closer look at a recent article on dental X-rays
Montreal, April 11, 2012
The Ordre des dentistes du Québec wishes to make a few points about an article entitled “Dental X-Rays and Risk of Meningioma”, published in the Cancer journal. Its conclusions have been widely reported by Quebec media recently.
The article, by epidemiologists from Yale University, concluded that dental X-rays could increase the risk of a meningioma, a benign brain tumour. The Ordre des dentistes questions the validity of some of the parameters in the study on which the article is based.
For instance, the researchers maintain that dental X-rays are the most common artificial source of exposure to ionizing radiation for people living in the United States, a form of radiation that is a known risk factor for certain brain tumours.
In fact, ionizing radiation associated with dental X-rays represents no more than 3% to 5% of the artificial radiation to which people are exposed, with the other 95% coming from medical X-rays.
The Order wishes to remind everyone that how often a person needs dental X-rays depends on his or her oral health and that the decision of whether or not to take X-rays depends essentially on the dentist’s clinical judgment, following an examination of the patient. Such decisions are never made in advance.
Remember that dentists are the only oral health professionals trained to make a diagnosis and establish a treatment plan. You should consult your dentist with any questions concerning your oral health.
– Supplementary information written by –
Denis Forest, DDS, MSD
Specialist in oral and maxillofacial radiology
Specialist in oral medicine
Results of the study which the article entitled “Dental X-Rays and Risk of Meningioma” is based on do not prove that there is a causal relationship between ionizing radiation associated with dental X-rays and the appearance of meningioma. The study shows at most a positive correlation.
Additionally, the number of dental X-rays administered to the people who participated in the study, who were between 20 and 79 years of age, could not be validated, because the researchers relied only on the individuals’ memory. In fact, clinical experience shows that patients have a very bad memory when it comes to estimate the number of radiographic examinations they underwent in the past and they have a hard time differentiating the different types of dental X-rays.
We can also question the methodology used in this study that indicates a positive correlation between retrocoronary (bite-wings) X-rays, panoramic X-rays and meningioma, but no significant correlation between the latter and full-mouth radiological examination, even though it requires from 15 to 20 X-rays, thus producing a radiation dosage at least 10 times higher than a retrocoronary X-ray.
On this matter, let’s highlight the fact that the tank containing the tube that produces X-rays in dental radiology is completely shielded and it must be verified by a physicist on a regular basis, who notably ensures that no leaks comes from the head of the machine.
As for the premises of the study that maintain that dental X-ray examinations are the most important source of artificial radiation for human beings, they are false, as shown with the following data.
Let’s remember that the human race has always lived in a world bathed in ionizing radiation. Human beings are subjected to two great sources of radiation: natural and artificial radiation. In total, these two kinds of radiation nearly account for about 360 millirems (mRem) per year for non-smokers and 640 mRem for smokers.
1. Natural radiation
Annual natural radiation comes from four main sources:
• Cosmic radiation coming from space, which equals to 26 mRem
• Terrestrial radiation issued from Earth’s radioactive elements, which represents 29 mRem
• Radiation issued from radon, radium and uranium, which sums to 200 mRem
• Internal radiation from food items, which accounts for 40 mRem
In total, the dosage from natural radiation is around 285 mRem per year (or 3 uSv per day), being 81% of total radiation received by the population on an annual basis.
2. Artificial radiation
Annual artificial radiation comes from several sources:
• Medical radiation during medical and dental radiodiagnostic examinations (38 mRem)
• Radiation issued from tests in nuclear medicine (14 mRem)
• Radiation issued from consumer goods – televisions, microwave ovens, phosphorescent dials, smoke detectors (11 mRem)
• Other sources, such as nuclear industry (2 mRem)
In total, the dosage from artificial radiation is around 65 mRem per year, representing 19% of the total radiation received by the population.
Individuals absorb a dosage of about 360 mRem of both natural and artificial sources each year, to those we have to add 280 mRem for smokers. We have to understand that natural radiation to which nobody can get away from is about four times more important than artificial radiation.
Dental radiation represents about 3% of artificial radiation: therefore they are not the most important source of artificial radiation, in opposition to what the authors of the study claim.
A simple rule to remember radiation exposure associated with dental X-rays is “10-10-100”:
• panoramic X-ray: 10 uSv
• cephalometric X-ray: 3 to 20 uSv
• 2 retrocoronary X-rays: 10 uSv
• 20 retroalveolar X-rays: 100 uSvSuch doses are considered very small.
On this matter, let’s evoke the position of the International Commission on Radiological Protection (ICRP), in the publication 105 of Annals of the ICRP, vol. 37, no 6, and entitled Radiological Protection in Medicine, as well as the notice from the American Association of Physicists in Medicine, who argue, about small doses, that it is not recommended to predict an increase in the risk of cancer on the sole epidemiological bases for people who receive doses lower than 50 mSv during a simple examination and 100 mSv for multiple procedures.
About dental radiology, dentists must always follow the ALARA (As Low As Reasonably Achievable) rule and remember that each radiological examination must be based on clinical judgement and be preceded by a diagnostic examination and a discussion with the patient.Dr Denis Forest
Press release from the American Association of Orthodontists (AAO)
Parents’ questions / Orthodontist’s responses
Why does my child need this X-ray?
The X-ray can gather information about your child’s condition that I cannot see with a visual clinical evaluation.
The X-ray will show the position of teeth that have and have not come in, and the relationship of teeth to bone and gum tissue.
Special X-rays also allow us to see how the jaws are related to each other and plan for properly directed treatment.
The information guides for diagnosis and treatment planning so that I can help your child achieve the best results possible.
Can diagnosis and treatment be effective without this X-ray? My child only has a few crooked teeth.
There is a science to moving teeth. The information gained through X-rays helps to know how to move teeth based on where they are now and where they need to be at the end of treatment.
Precise position and placement of teeth can only be assessed through X-ray images. This aids the diagnosis and treatment planning to deliver the best results possible for your child.
Which type of X-ray will provide you with the information you need with the least amount of radiation exposure for my child (routine X-rays, panorex or cone beam CT)?
A cone beam CT (CBCT) provides far more information for diagnosis than routine retrocoronary (bite-wings) X-rays or retroalveolar (periapical) X-rays, a panoramic X-ray or a cephalometric X-ray alone.
However, not all patients require a cone beam CT. Not all orthodontics clinics have tridimensional CBCT machines. The majority of diagnoses are made with cephalograms and panograms. A 3D CBCT can be converted into a 2D image.
The recommendation for the type of X-ray needed is based on each child’s individual needs. Based on current science and our clinical experience, we strive to match our diagnostic imaging with your child’s needs. Our goal is to maximize the benefits and minimize the risks to our patients.
Retrocoronary X-ray
The American Association of Orthodontists recommends taking retrocoronary (bite-wings) X-rays of left and right posterior teeth and retroalveolar (periapical) X-rays to detect periodontal diseases in adults who must receive a major orthodontic treatment.
Crowns of upper and lower teeth can be seen on a retrocoronary X-ray and this X-ray offers a direct view of the interproximal bone level.
On the left X-ray, arrows 1, 2, 3 indicate the bone level. Arrows 1 and 2 point toward sites where bone loss is located between the second premolar and the first molar and between the first and second molars (teeth 26-27). Arrow 3 indicates a normal bone level. Arrows 4 and 5 indicate the presence of unerupted third molars.
Back to top
Retroalveolar X-ray
A retroalveolar X-ray shows the teeth in their full dimension, including the end of the roots. On the X-ray #1 where we can see from left to right a canine, a lateral incisor and a central incisor, arrow 1 indicates where the interproximal bone should be and arrow 2 indicates where it is located in reality. The difference in height between both arrows indicates the bone loss. This patient presents a moderate chronic periodontitis of sites 11-12 (X-ray #1), 26-27 (X-ray #2 and retrocoronary X-ray above) and 16-17 (not shown).
X-ray #3 represents the same patient’s lower right posterior teeth. Arrows 1 and 2 show acceptable bone level. The number 3 in the radiopaque (white) part on the tooth represents an obturator made of composite material (white filling).
Back to top
Panoramic X-ray
A panoramic X-ray or panogram represents an entire view of the maxillary and mandibular dentition and the temporomandibular joints, maxillary sinuses, the nasal septum and lower turbinates.
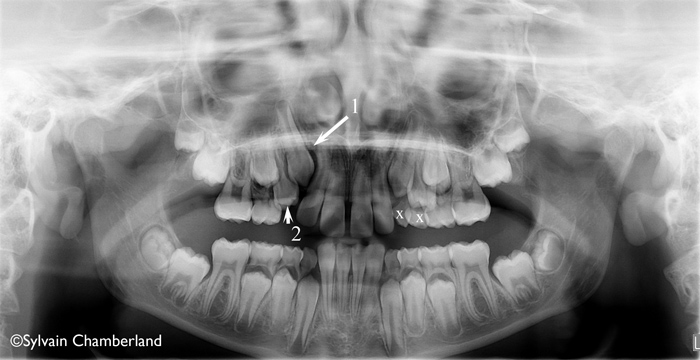
On this X-ray, the upper right canine (arrow 1) does not have sufficient space to erupt between the premolar (arrow 2) and the adjacent lateral incisor. The sequence of eruption is not symmetrical, because the primary canines and the right first primary molars have exfoliated whereas it is not the case on the left side (teeth marked with an “X”). To balance the situation, we have prescribed the extraction of the primary teeth marked with an “X” and the patient will be re-evaluated in a year.
Cephalometric X-ray
A cephalometric X-ray or cephalogram represents a lateral view of the face. It enables us to see the relationship between the jaws with regard to the base of the skull and the relationship of the lower jaw compared to the upper jaw. It also enables us to evaluate the position of the teeth compared to their respective jaw and the relationship between the upper and lower teeth. The position of the lips is evaluated with the tangent line between the nose and the chin (blue line). On this cephalogram, there are several numbers used by the orthodontist to quantify the relationship of teeth and plan their direction of movement like he quantifies and plans the position of the jaws.
Back to top
Cone beam computed tomography (CBCT)
A computed tomography brings a 3D view. A CBCT contains a lot of information and allows for very precise specific examinations of the skull or more specific areas, such as the temporomandibular joints.
The CBCT shown on the opposite side was prescribed to evaluate how severely arthrosis affects the left temporomandibular joint. The right side presents a normal condyle and a normal neck of condyle. The left side shows a condyle resorbed by arthrosis. The neck of the condyle is shortened because the upper part has “melted” because of arthrosis. This patient has severe idiopathic condylar resorption.

CBCT right lateral view. (Courtesy of Marie-Hélène Cyr)
I recommend you visit the mhcyr.com site. She is a passionate young lady who tells the story of her orthodontics-surgery experience with a large number of details. You will find her complete story. I promise you interesting hours of reading.
She even displayed images of her skull obtained by a CBCT.
It is probably the best site and blog created by a person who is not an orthodontist and who wishes to publish information of high quality.
Back to top
Do you use faster E- or F-speed film for X-rays? The New York Times article says that “D” speed film is too slow and causes my child to get too much radiation.
We only use digital images which help reduce radiation dosages.
I don’t want my child to have any kind of X-ray. Can’t I just sign a waiver of some kind?
No. X-rays are necessary for me to diagnose your child’s orthodontic problem and plan the right treatment to correct the problem.
How do I know how much radiation my child will receive from this X-ray?
My X-ray/panorex/CBCT machine’s standard dosage is computer-controlled. The machine is calibrated by me or my staff for each patient depending on his or her body size (height and weight) and age. The ICRP (International Commission on Radiological Protection), an organization that sets standards to protect the public, recommends limiting non-occupational exposure to ionizing radiation to 1,000 pSv per year. The exposure your child receives remains a fraction of that dosage.
Will you put a lead apron, thyroid collar or other shield on my child to avoid unnecessary exposure?
The lead apron is put on every patient without exception.
What kind of training do you or your staff have to administer an X-ray?
Training varies with the type of equipment. Companies that make X-ray equipment provide in-office training at the time of installation, and updates the training as required by new technology that’s applied to my equipment. Additionally, there is in-office training on new equipment as needed.
Is there a provincial or federal inspector that makes sure the X-ray machine is not emitting too much radiation?
It is mandatory to have the equipment and the room where the equipment is installed verified by a physicist. An evaluation is necessary every 3 years and we have to send this evaluation report to the Laboratoire de santé publique du Québec for the renewal of the license for operation of diagnostic X-ray equipment. We use services provided by the company called Radioprotection Inc. accredited by this same laboratory.
Does research show how much radiation it takes to cause cancer?
There are no reports of illness caused by dental X-rays.










Many diseases of the oral cavity can’t be seen when the dentist examines your mouth. Dental x-rays are images that can help the dentist see things the human eye can’t detect, such as tiny areas of decay between the teeth and the position of unerupted teeth in children and adults.
“In total, the dosage from natural radiation is around 285 mRem per year (or 3 uSv per day)”
285 mRem = 2,850 uSv per year
2,850 ÷ 365 days = 7.8 uSv per day.
I think it should 7.8 uSv per day.
Thank you so much with this great topic. I learned alot. Have a happy new year!
Thank You Dr. Vu for the precision about the dosage of radiation
However, the supplementary information of Dr. Denis Forest say:
The radiation we are subjected is from 2 sources: natural and artificial.
Therefore, the dosage of 360 mRem is likely greater than the dosage from natural radiation of 285 mRem.
You may be both right.
Best regards,