Impacted canines and root resorption of the incisors
Question :
Hello Dr Chamberland,
My 12-year-old daughter Lorène has both impacted upper canines. After consulting an orthodontist, she recommended the removal of both deciduous canines to make room for them to erupt but they did not come out. The treatment started a few years ago already. They first tried to make room for the canines with an appliance.
After a panoramic picture, here is what she proposes (she is talking to my dentist):
“We must make a decision for little Lorène concerning the impacted teeth #13 and #23.
Of course and this is beyond a doubt, generally, if traction can be used on canines, the adequate treatment is de-impaction and traction of these teeth.”
With Lorène, we have already discussed it with doctor XXX (stomato), the situation is different and quite delicate. Indeed, and you will see it on the pano, the follicular envelope of teeth #13 and #23 (but mostly teeth #13) has resorbed the root of teeth #12 and #22 with teeth #12 that is mobile and really in a risky situation.
Our question is: in this very particular case, wouldn’t it be wiser, to avoid more trauma on the laterals, to extract teeth #13 and #23 and perform a loss of anchorage and coronoplasty of teeth #14 and #24 with aiming for having the group of premolars act as canines?
We went to see another orthodontist who confirms that the impacted canines indeed resorbed the lateral incisors and even the central incisors… and who confirms the diagnosis.
What do you think? Is it really the best solution?
Thanks in advance,
Eric Lacasse
Attachment: Panogram
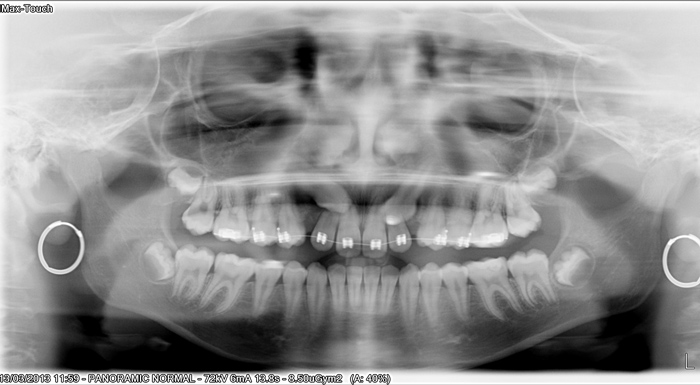
Réponse :
Good Sunday morning Mister Lacasse,
It is true to say that the situation is quite bothering and that damage to the permanent teeth is present.
You daughter is 12 years old and you say that the treatment started “several years” ago. This confuses me.
I think that there is a strong iatrogenic cause to the resorption of your daughter’s incisors. The problem should have been handled way before and differently. It would have been better to de-impact the canines first (exposure surgery, traction metal ligature and removable appliance with a cantilever spring) WITHOUT using fixed appliances. When traction was performed on the canines, it would have been simple to make the decision to undergo a major orthodontic treatment and to proceed with the removal of premolars to solve the problem of the lack of space. All of this assumes that the canines were accessible by the palate.
But the damage is done. The same option can be considered. I would certainly remove the fixed appliances to free up the lateral incisors during the traction of the canines. As soon as the crown of the canines will be moved away from the root of the lateral incisors, the root resorption will stop, healing will follow and the treatment with fixed appliances will be able to start again.
What now?
The option to extract both canines is a good choice. It is probably what is simplest mechanically and as soon as the canines are gone, resorption will stop. The first premolars (#14, #24) can fill out the role of the canines with or without coronary modifications. I am thus in favor.
Note that the removal of the lateral incisors would not be a bad choice, but the duration of treatment will be longer, because the canines need to be brought into the mouth and this can take one year or even more. By seeing how the canines were managed up to now by the orthodontist, I would be careful…
What calls to my mind is that nobody talked to you about the definitive relationship between the upper and lower teeth. Indeed, there will be 2 fewer teeth in the maxilla and a complete dentition in the mandible. A treatment with the extraction of 2 teeth in the maxillary arch is valid if the molar relationship is in Class II. If the molar relationship is in Class I, we have to consider the removal of 2 lower premolars to obtain an acceptable functional occlusion.
I introduce you to a case of a patient who comes to my office and who has 2 impacted canines that cause resorption of the incisors. Any traction attempt on the canines would have meant a more important damage to the incisors. The patient had a Class II malocclusion. I thus proposed a treatment including the removal of 2 permanent maxillary canines, but without any removal in the mandible. Notice that the treatment was initiated in the mandibular arch while waiting for the upper canines to be extracted. The treatment in the maxillary arch started in March a few weeks after the extraction surgery. Notice the resorption of teeth #21 and a little bit of teeth #22. Teeth #12 and #11 are less damaged.

I forgot to ask you if braces on the maxilla are necessary. The orthodontist who wanted to extract lower premolars said that the braces were obviously necessary on the mandibula but absolutely not on the upper part as the traction will damage an already touched lateral incisor. Thank you. Sveta.
Yes, braces in both arches are necessary.
I would like to attach a few images to clear the situation. The maxillar canines were extracted with success.
Now my dentist wants to extract a lower lateral incisor, put on the braces and also use the braces on an upper arch.
Will it damage even more the lateral incisor with reabsorption?
Another dentist had an idea to extract two lower premolars, use braces and do not use them on the mandibular arch.
What do you think about that?
Thank you very much in advance.
Sveta.
Hi Sveta
This post will cover the question at 16 h23 and 19h57. Thank you for sending me the picture to my professional facebook page.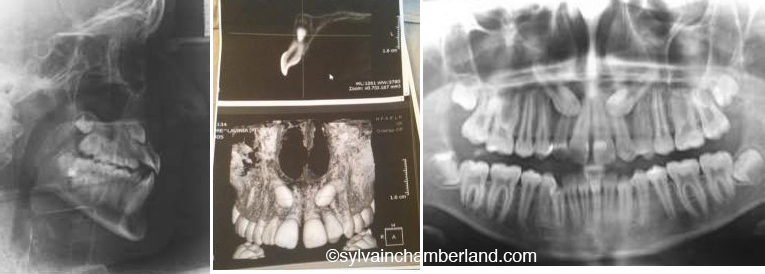
The ceph show a class I relationshipm normal overjet and overbite. The 3D view shows the lateral incisors buccaly overlayed on the roots of the lateral incisors. The pan and the significant lack of space. I can see crowding of the lower right canine.
On september 24, my recommendation #1 was extracting both upper canines and 2 first lower premolars.
Since the canine are extracted, it is a little bit too late to discuss a non extraction apporach.
I am not confortable with extraction of 1 lower lateral incisor. It may be difficult to obtain a nice functional occlusion.
I would prefer the option #1 as suggested in september.
I would not worry that much about further root resorption as the cause has been removed and if the orthodontist let it healed 6-8 weeks.
By the way, you mentionned dentist being the care provider. I strongly recommend that you visit a certified orthodontist for the treatment of your daughter.
I hope that help.
Best regards.
Dr Sylvain Chamberland.
Thank you very much for such a fast reply. My dentist shares his studio with an orthodontist, they usually work together. The decision to extract a lateral incisor was actually hers. Another orthodontist offered your type of approach and honestly I feel more comfortable with it. Do I need to make a new X-ray and 3D? Thank you. Sveta.
I would not take a new 3D, but I would take a new ceph, a new panoramic xray, new intraoral and extraoral photos.
Hello Dr Chamberland,
My 13-year-old daughter has 13 and 23 canines included, the root of 12 incisor is slightly damaged. We consulted a few orthodontists and came to no real conclusion. Some one them offer extracting 13 and 23 and the premolars in the mandibular arch, others think that traction of the canines with extraction of premolars is the best idea. One of them offered to extract the lateral incisors and track the canines there. My daughter is unfortunately class 1. Does it necessarily mean that the mandibular premolars must be extracted?
It is not unfortunate to have a class I occlusion. Indeed, it is very fortunate.
Both tx plan can be valid.
1- I mean if damaging further the root of the lateral incisor, it is a reasonbable plan to extract both maxillary canines and 2 first lower premolars.
2- It is also a good option to pulls the canine, make sure it move adequately, then extract 4 first premolars, continue to bring the canines in and close all extraction space.
3- Extracting both upper lateral incisors and lower 1st premolar could be an option, but only if there is severe damage to the root of the lateral incisors.
I have done all 3 options of treatment in my career.
If she is class I and that extraction are necessary in the maxilla, then extraction in the mandible is unavoidable.
Sometimes it is possble to do it non extraction if there is minimal if any crowding in both arches.
I hope that help.
My daughter had her surgery 3 weeks ago. It seems like everything went well. As I mentioned before, her 12 tooth root was actually damaged by 13 laying position. Now it has an open part of the root. Is it necessary she has to extract its nerve in the future?
I asked a dentist if he could cover it right after the surgery and he said no. How long does it take to place the brackets after surgery?
Is it safe to wear them on a damaged tooth?
I made a huge mistake above. My daughter is class 3.
Almost 2 months after surgery her upper incisors are doing very well and seem to be in a good position, much straighter than before. Our dentist thinks that extracting one lower lateral incisor and outing on the brackets could save the situation. It seems quite weird to me.
Actually my daughter chews more like an old person without teeth.
Her mandibula is rather forehead. What do you think about this situation?
Thank you very much in advance.
Hi Sveta
I will try to cover you 3 questions.
When the canine were extracted, the surgeon is supposed to recover the root of the remaining incisors. The roots should not be exposed.
In term of root canal therapy, I would absolutely not recommend it. Let the roots of teeth healed and the surronding bone regenerate.
I would wait 6-8 weeks before moving the teeth with brackets and wire.
hi,would you please give me some evidence about leaving the root to heal by themselves instead of doing RCT ?? I’m an endodontist and i’m searching fore evidences in this field,but unfortunately i don’t have access to any of the studies in this field
The cause of root resorptionin such case is the canine that is damaging the root as it erupt. It is a well known and accepted fact that once the canine is moved away from the root, the resorption stops. External root resorption is a very different problem than internal root resorption where the cause of the resorption come from the pulp.
I hope that help.
Hello Doctor Chamberland,
Here are news on Lorène.
This time, this is it… The orthodontist will try to go get the canines. It is a real art… He will first remove the 2 external incisors (which will anyway fall out in the short term since the roots are damaged). Then, to go get the impacted canine, he will move the incisors on the side and pull on it. He will try to save at best the main incisors (but they are, according to him, also doomed in the medium term, because they have also resorbed to a lesser degree and one more than the other. We will see…) The canine which is in the palate will be pulled backward in the meantime. He will then put everything back where it belongs… It is complex but the goal is to save the canines which are healthy teeth while the incisors are doomed in the medium and short terms. Lorène should undergo two surgeries under local anesthesia.
This seems to me like the best that we can do. I am happy to have stopped beating about the bush and a little calmed down even if we are in for a heavy treatment. Thank you for your advice.
Regards,
Eric Lacasse
I am happy to learn that you are going ahead with a solution that seems OK to me. I would like to reassure you about the central incisors that have resorbed. Know that as soon as the canines are no longer near them and stop putting pressure on them, the resorption will stop. So even if 3, 4, 7 mm of roots have resorbed from the central incisors, once the treatment is over, this does not mean that these teeth have a worse long-term prognosis. She can live with this all of her life like we say back here.
I imagine that your orthodontist has put appliances in the mandibular arch to match both dental arches. Otherwise, there is another problem that will get to you sooner than later. You wrote on 8 December that she had a Class II relationship. This is compatible with an orthodontic treatment where 2 teeth in the maxillary arch are extracted (the lateral incisors in Lorène’s case).
Canine lateral substitution and Class II molar relationship.
I show you an example of a treatment where the missing lateral incisors were substituted by canines and there is a Class II molar relationship. There were no extractions in the mandibular arch.
As far as the lower arch is concerned, it is favorable, my daughter is in Class II.
Regards,
Eric
I am very happy to learn that one of the canines has erupted by itself. I assume that it is the left one because its position seemed less problematic on the panogram.
A CBCT will allow defining the position of the impacted canine relatively to the roots of the incisors more precisely.
The fact that a canine is in the mouth changes everything. A different treatment plan can be considered. This treatment plan must include treatment of the mandibular arch, the likely lack of space in the maxillary arch and the fact that the roots of one or two incisors have resorbed to the right and the feasibility of bringing the impacted tooth into function.
I do not see any problems keeping both canines, but the right canine needs to be taken away from the incisors to stop the damage. This should have been done a long time ago. The problem is that there is no global approach for the maxillary arch as well as the mandibular arch.
A lot of time was wasted by a lack of understanding of the case and the inherent risks to the impacted canines.
Good luck
A CBCT is a lot more serious to help in diagnosing an impacted canine and its relationship with nearby structures. To see examples where this imaging technique was a precious diagnostic help; follow this link
Homeopath???? I quite laughed. I am a mechanic and I am one of Dr Chamberland’s patients. And there is no use in having a degree at university to know that a homeopath cannot do anything for your daughter’s teeth. Apart maybe from wasting your young daughter’s time.
When I work with a new young mechanic and he tells me that he does not understand an electrical problem, I tell him that he can continue believing that it is magic, or consult the technical publications and understand the problem. On the same level, I do not believe that a phoney homeopath can move teeth…
Mister Dufour, you are a practical guy. No fooling around.
LOL, I would not hesitate to get my car repaired at your garage!
Hello Dr Chamberland,
Thank you so much for your response which is clear and understandable. I forwarded it to our orthodontist to see her reaction…
It is possible that when we contacted her the first time, I do not quite remember when it was, it was maybe already too late to apply traction to the canines in the palate… but anyway, the appliance she wore to make room was frankly useless… as you say, the damage is done.
We were also told about a very thin permanent wire to fix behind the incisors to consolidate them (I do not remember the exact term). What do you think about the use of this appliance?
Thank you in advance,
Regards,
Eric Lacasse
The permanent wire that you were told about is a wire bonded to the lingual side of teeth. I put this kind of wire routinely in the majority of patients when I remove their fixed orthodontic appliances. No need to have root resorption. The goal of this bonded retention wire is to preserve alignment of teeth. Of course, if one or more teeth are weakened by exaggerated resorption (50% or +), this can be useful to solidify the tooth.
Thank you for keeping me in the loop
Hello Doctor Chamberland,
Thank you again for your response and your interest in our case. To be honest, my spouse and I are confused…
We do not “feel” the extraction of canines at all – surgical procedure that will probably be quite traumatizing to our daughter who has just already worn an appliance for 3 years…
I talked to a friend about it and she advised me to make an appointment with a homeopath, which I did.
Regards,
Eric
Wow!
A homeopath? Why not walk on Compostela road? Or eat bananas? Or ask Santa Claus? A shaman maybe?
Or ask Santa Claus? A shaman maybe?
I have a colleague who made this recommendation on his site about someone who was looking for a miracle method to close an interincisal diastema. He thinks that it could work for impacted canines as well… Maybe homeo banana pills would kill 2 birds with one stone.
I believe that you do not understand how severe the situation is. You daughter’s condition which seems to have been managed so-so up to this date (rather poorly than well), what on earth will a homeopath, who has no dental training, no knowledge of the evolution of dentition, do better with imposition of hands and a banana pill?
In your daughter’s case, it takes a cone beam computed tomography to determine the extent of the damages and the real position of the canines. In the above example, you can see the root resorption of the upper incisor and how close the crown of the canine is to the root of the incisors. It is another example where the therapeutic decision included the extraction of 3 premolars (#14, #34, #44) and the impacted canine (#23). With this being said, do not believe that I only do that, extract impacted canines. I show you exception cases, because the rule is rather to spare the canines.
I told you so. It is not necessarily impossible to apply traction to your daughter’s canines. However, it will take space in the dental arch to put them and it is not simple. Extractions will likely be necessary. It could be #14 and #24, it could be #13 and #23, it could be #12 and #22. I told you that a treatment will need to be done in the mandibular arch and as there will be extractions in the maxillary arch, extractions will likely be required in the mandibular arch unless a Class II relationship exists.
I wish that you would consult a certified orthodontist who will present to you a comprehensive treatment, without compromise rather than a partial solution. The stomato only does surgery, he does not know orthodontics much if at all.
I spent a lot of time answering you the best I could.
But a homeopath… I cannot believe it.
If a homeopath can move these impacted canines and position them in the dental arch, we invite him to the Quebec Association of Orthodontists to allow him to teach us how to do it, I will be all ears!
Hello Doctor Chamberland,
We went to see the homeopath who recommended that we go see a colleague homeopath/dentist who just recommended to us to go for a cone beam computed tomography…
We will go next Wednesday…
In the meantime one of the canines came out in the palate, the other one is still hidden…
I will keep you informed,
Regards,
Eric